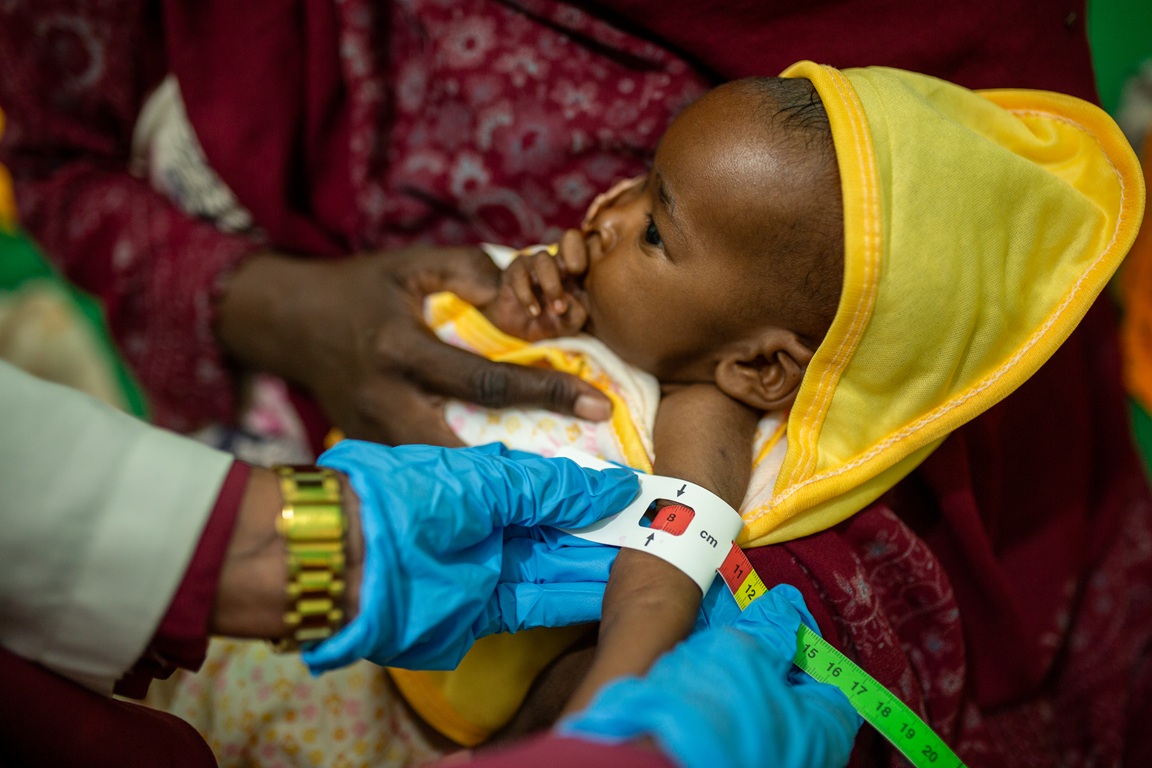
Beyond the Virus: What mpox taught us about people, evidence and response
%20(3).png)
By Dr. Gillian McKay, Head of the Humanitarian What Works Centre, Elrha
In 2024, as mpox spread across Central and East Africa and beyond, it became clear, once again, that outbreaks are not just about pathogens. They are about people: how communities understand risk, how they seek care, and how trust shapes every aspect of response.
At Elrha, we knew we had to leverage our funding to address the outbreak, but it was this recognition that most shaped our approach from the outset. While large-scale biomedical research on vaccines and therapeutics was already underway, we identified a critical gap: real-time evidence on how communities were experiencing mpox, how they were engaging with response efforts, and what response actors could do to make the response operation more people-centred.
Through a rapid scoping of evidence needs, we chose to fund a portfolio of social and behavioural science studies designed not just to generate knowledge, but to inform response as it unfolded. Our recent webinar Beyond the Virus: Social and Behavioural Science Lessons from Mpox, brought together researchers, practitioners, and policymakers to reflect on what we have learned from that portfolio, and what must come next.
Across all speakers, a simple but powerful message: outbreak response is only as effective as it is socially informed.
From evidence to action in real time
A defining feature of the work presented was its embedded nature. These were not studies conducted at a distance; they were designed and delivered within response systems, in partnership with Ministries of Health, national researchers and research institutions, and community organisations.
This was intentional, as we prioritised research with a clear uptake pathway, ensuring that findings would feed directly into operational decision-making, not just an academic article (though of course these are essential for long-term knowledge!)
In one study in Tshopo Province (DRC), rapid qualitative research was conducted in just seven days, generating actionable insights on community perceptions, trust, and care-seeking across seven domains of community protection. Crucially, findings were taken back to communities to validate recommendations, and then directly into response coordination structures, resulting in concrete outputs such as integrated communication strategies and implementation plans.
Across multiple projects, the message was consistent: timely, operationally-relevant research can shape decisions, not just document them.
Communities as partners, not participants
A second clear thread was the shift from viewing communities as ‘beneficiaries’ to acknowledging and celebrating them as active agents in research and response.
In Kinshasa’s Pakadjuma neighbourhood, the research team worked with people who had recovered from mpox to co-develop public health interventions and to form a formal association for ongoing livelihood opportunities. These recovered patients became trusted intermediaries for the mpox response, bridging communities and health systems, reducing stigma, and reaching populations often excluded from formal health services in this highly marginalised geography.
Similarly, peer educator models helped engage at-risk groups, such as sex workers, men who have sex with men, and highly mobile populations like truck drivers, both in research and in response efforts. These approaches not only improved data quality but also strengthened trust and engagement with the response (and in some cases even helped identify and refer mpox patients to care).
Perhaps most strikingly, community-led structures developed through the research continued to operate beyond mpox, supporting responses to other outbreaks such as cholera, demonstrating lasting resilience and capacity.
Context matters – always
Across studies, one of the most consistent findings was that mpox is experienced differently across contexts.
Knowledge, risk perception, and vaccine acceptance varied significantly by geography, population group, and social context. In some cases, even among high-risk groups, awareness of mpox was limited. In others, structural barriers, such as poverty, stigma, or lack of access to services, made it difficult for people to follow public health advice.
This reinforces a core principle of social and behavioural science: there is no one-size-fits-all response. Effective interventions must be grounded in local realities, shaped by lived experience, and adapted continuously as outbreaks evolve.
Ethics, trust, and participation
The webinar also highlighted the importance of ethical, participatory approaches, particularly in emergency research.
Work adapting a good participatory practice toolkit from Ebola for mpox showed how equipping communities with knowledge of their rights can transform engagement. When people understand the purpose of research, their role within it, and their rights as participants, trust increases, and so does the quality of evidence generated.
At the same time, communities emphasised that engagement must go beyond consultation. As one participant reflected, involvement must start from the beginning, shaping priorities, not just responding to them.
From research and response
A recurring theme was the persistent tension between the speed of response and the time required for research.
Encouragingly, progress is being made. The development of a generic, pre-approved community assessment protocol for social and behavioural science now allows rapid qualitative data to be collected, analysed, and used within days or weeks. These tools have already been applied across mpox, Ebola, and cholera.
But tools alone are not enough. To fully close the gap, we need:
- Pre-positioned systems (funding, ethics, partnerships) that can be activated quickly
- Stronger demand from decision-makers for social and behavioural evidence
- A shift in mindset, recognising operational research not as “less than” academic research, but as something essential and just as valid
What comes next?
Looking across the portfolio, what emerges is not a single study, but a mosaic of insights – exactly the kind of layered, real-time evidence we set out to generate.
Together, they point to a more effective model of outbreak response, one that is:
- Embedded in response systems
- Led with communities, not for them
- Grounded in context and lived experience
- Designed for real-time use
There are still important research gaps to address, from understanding care outside formal systems, to the experiences of marginalised groups, to the longer-term impacts of mpox on recovered patients.
But the direction is clear, as we face an increasing number of health emergencies globally, investing in social and behavioural science is not optional, it is essential. Because ultimately, outbreaks start and end with people and communities. And if we want responses to be effective, they must start and centre there too.
Watch the webinar recording
Stay updated
Sign up for our newsletter to receive regular updates on resources, news, and insights like this. Don’t miss out on important information that can help you stay informed and engaged.
Explore Elrha
Learn more about our mission, the organisations we support, and the resources we provide to drive research and innovation in humanitarian response.