Key insights for humanitarian policy and practice from our COVID-19 research
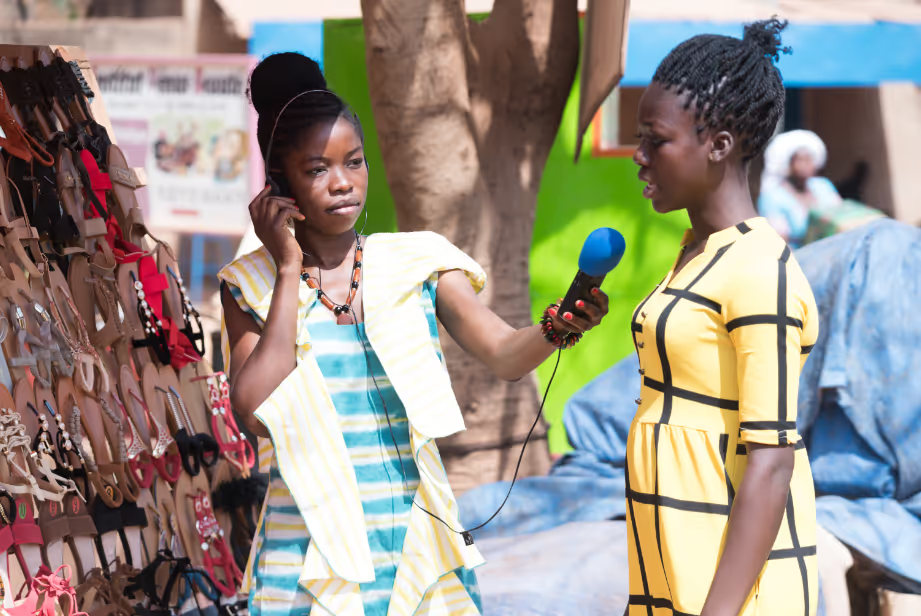
The ongoing COVID-19 pandemic has prompted global demand for rapid research to understand the dynamics of the outbreak, and its impact worldwide.
This demand was particularly urgent in humanitarian settings, where local data was not readily available, and where certain groups, including refugees and internally displaced people (IDPs), may have been at higher risk.
In March 2020, within weeks of the WHO declaring COVID-19 a pandemic, we used the responsive research mechanism of Elrha’s Research for Health in Humanitarian Crises (R2HC) programme to launch a call for COVID-19 research. By June, 15 studies were active in 13 countries, all selected for their potential to contribute critical evidence to the COVID-19 response in humanitarian settings.
We recently convened a conversation between some of these researchers and humanitarian practitioners to explore what the research tells us about COVID-19 in humanitarian settings, and specifically for refugees and IDPs.
Here were some common insights and issues relevant for policymakers and practitioners.
1. Locally tailored approaches ensure effective public health interventions
Gaps between “top-down” public health policies and guidelines and local practices are widespread.
A research team led by researchers from Michigan State University studied the implementation of one humanitarian NGO’s safety protocols. They found cultures of adherence — or lack of adherence — developed around particular policies in different locations.
While certain actions, such as physical distancing and mask-wearing, were promoted as effective preventative measures, sustained engagement with communities and local engagement and adaptation have proven critical to ensure adherence to public health recommendations.
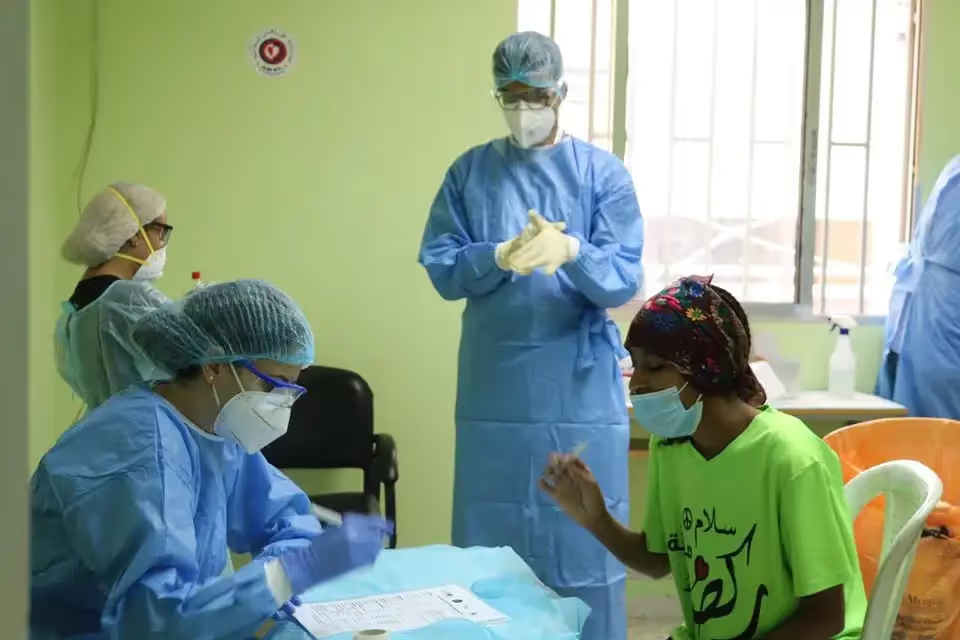
Unsurprisingly, broader concerns related to livelihoods and food insecurity had taken precedence in many places, superseding intentions to abide by public health guidance. Food insecurity among refugees was a theme in several studies in settings as varied as Gaza and Uganda, leading one study team to title a policy brief ‘What will kill refugees first — COVID-19 or hunger?’
This is particularly important as efforts to control the spread of COVID-19 coincide with growing concerns related to other health, social and economic needs that have been deprioritised in favour of immediate pandemic response efforts.
The same study in Gaza noted that rising debt levels and depression are a concern among certain communities, while a study in Colombia found that both locals and Venezuelan migrants have sought less care from health services, partly for fear of catching COVID-19.
2. Getting communication right is critical
Scepticism and misinformation have further complicated the public health response in several countries, with R2HC-supported research revealing high levels of scepticism related to COVID-19 and its potential harm.
While most R2HC-funded studies have so far reported reasonably good awareness of COVID-19 symptoms and transmission risks among refugees and IDPs, there are also some worrying gaps, including low awareness of asymptomatic transmission, or the perception among humanitarian staff that there is not the same need to physically distance when with their colleagues than with refugee camp residents.
Rapidly changing knowledge of COVID-19 may be partly responsible.
During our panel discussion, Mohammed Al-Zayed from Amel Association International noted that a huge volume of information has led to protocols and guidance changing overnight, making it hard for practitioners in Lebanon to keep up with the latest recommendations.
A more detailed understanding of levels of awareness, and the reasons people give for their scepticism and misunderstanding, has helped inform public health programming in real-time, including the development of locally contextualised public health messaging, and a greater focus on who is targeted and how.

In Uganda, radio is a popular source of news and information whereas in Gaza social media has been useful with the engagement of youth activists.
Meanwhile, a study team in Lebanon has produced simple, animated Arabic videos that health responders can distribute to raise awareness of COVID-19 infection risks among older refugees.
Taking the time to get to know different audiences, and how and where they obtain news, has generated valuable knowledge that has improved the quality of health messaging, This echoes lessons learned by study teams we fundedduring the Ebola response.
While many studies have focused on adherence to early preventative measures, vital information has also been gathered related to vaccine acceptance and uptake, which will be critically important as global vaccine roll-out gathers pace this year.
For example, researchers in Lebanon found very few older people were planning to register for the vaccine, prompting a need for improved risk communication to promote the vaccine and increase registration.
3. Community engagement is key
Close collaboration between researchers, humanitarian organisations, government ministries, other local actors, and communities affected by COVID-19 is essential to ensure an effective public health response.
Reflecting on the benefits of an Elrha-funded research collaboration with researchers at Kampala’s Makerere University, Ugandan Ministry of Health representative Brian Luswata emphasised the value of policy-making driven by evidence gathered with communities at the local level.
In Jordan, one study team led by the International Rescue Committee has proposed that greater attention is paid to the role of community health volunteers as a strategy to reach refugees with chronic diseases in order to minimise the impact of COVID-19 on access to healthcare.
Research and programming must also identify approaches that look beyond the narrow focus on COVID-19 to incorporate other pressing health and socio-economic issues, many of which may present a far greater concern to certain communities.
It is clear the social and behavioural sciences — again, as exemplified during the Ebola response — can help us listen to, and engage with, diverse communities and strengthen their agency as key stakeholders in decision-making that affects them.

4. COVID-19’s impact on humanitarian response is long-term and broad
For operational health and humanitarian responders, COVID-19 continues to present a huge challenge, both in relation to the direct burden of disease and the indirect impact of the pandemic on essential supply chains, the availability of staff and materials to ensure their safety while working, and the diversion and reduction of funding for other essential programmes.
During our panel discussion, humanitarian staff with direct experience responding to COVID-19 reflected on the ways in which the pandemic response has changed over the last 12 months.
While there was an early need to gather knowledge of the virus and how to prevent its spread, concerns have shifted to how best to adapt to living with the ongoing impact of the pandemic.
This impact is not limited to the physical harm posed by COVID-19, but also the disruption of almost all aspects of day-to-day life.
5. The world must affirm humanitarian priorities
In many humanitarian contexts, delays accessing routine care for other medical problems, as well as growing mental health needs and major protection concerns, particularly in relation to the significant increase in gender-based violence, have placed pressure on health and humanitarian organisations.
In some cases, this has required the difficult task of prioritisation between the most immediate needs. Moving forward, ensuring protection for the most vulnerable must remain high on the humanitarian political and funding agenda.
As MSF Migration Advisor Aurelie Ponthieu noted, the pandemic response has been heavily politicised, with the imposition of restrictions and border controls that have often exceeded their public health justification.
For people living in camps and border areas, and those attempting to flee conflict and violence, these measures pose a major threat to health, wellbeing and human rights.
Many of these concerns, and findings from early COVID-19 research, raise yet more questions that require further exploration in the months ahead, while questions related to the long-term direct and indirect impact of COVID-19 will likely form the basis of many research collaborations for years to come.
More immediately, as global vaccination efforts gather pace, the urgent questions of how to address vaccine scepticism and other barriers to uptake, and enable and support access to vaccines for people in humanitarian settings, must be a collective priority.
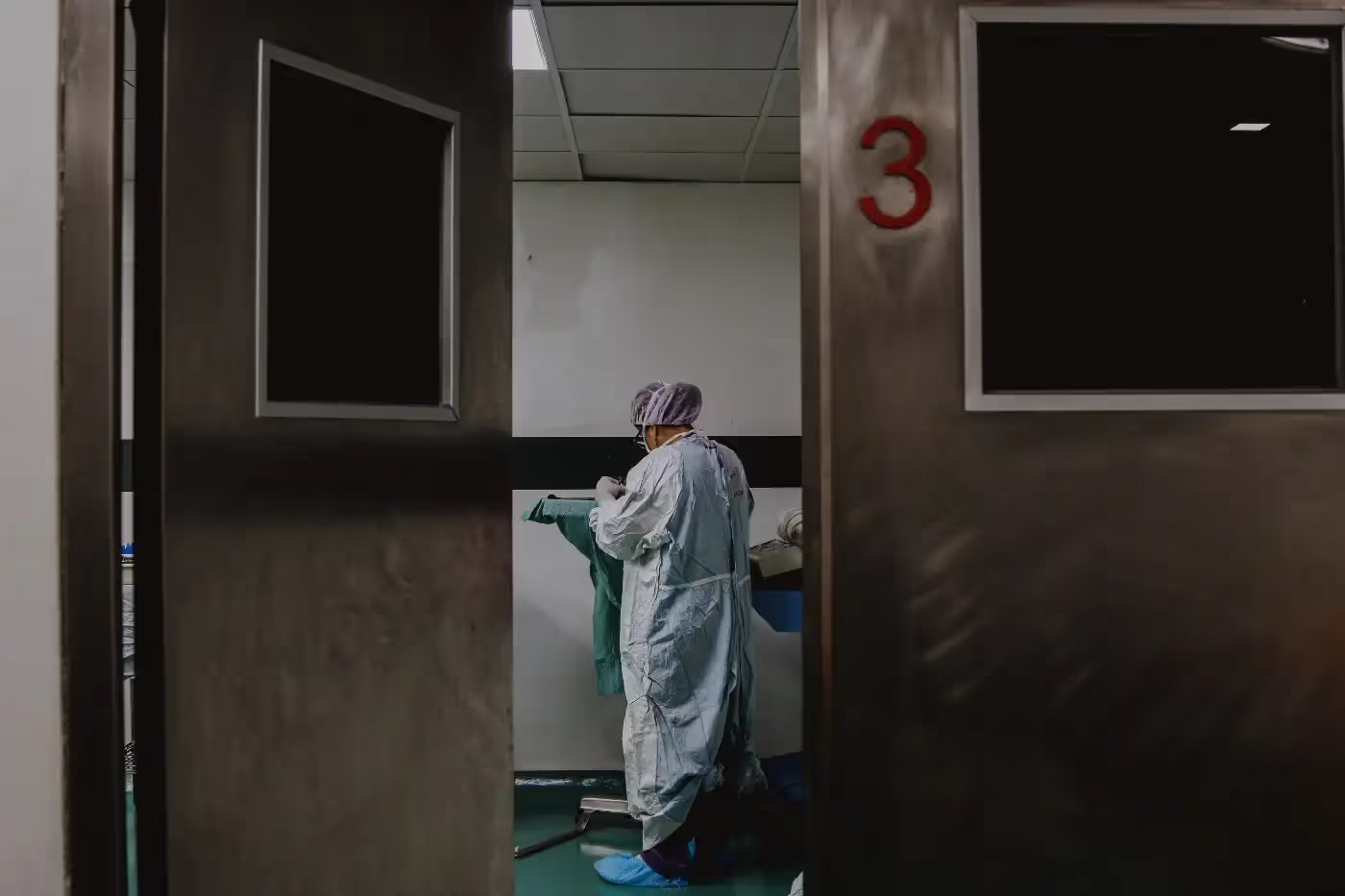
The continued importance of research
We are confident that timely and relevant research, developed in partnership with local communities and other stakeholders, has the potential to inform effective and locally appropriate humanitarian health response. But research can only do so much.
Evidence must be applied, shared, and translated for practitioners. Effective, evidence-informed interventions must be funded, and most importantly, the needs of communities must be recognised and taken into account — both during the research process and during the implementation of programmes.
As more of our COVID-19 studies generate knowledge, we will continue to share what is being learned by researchers, humanitarian organisations and communities to inform the ongoing global response.
For more about the rapid research projects Elrha has supported, visit here.
Stay updated
Sign up for our newsletter to receive regular updates on resources, news, and insights like this. Don’t miss out on important information that can help you stay informed and engaged.
Explore Elrha
Learn more about our mission, the organisations we support, and the resources we provide to drive research and innovation in humanitarian response.