Making space for palliative care in humanitarian action: Reflections on obstacles to the integration of palliative care approaches in humanitarian healthcare
Many situations arise in humanitarian crises when curative care is not the primary, or the only, mode for humanitarian healthcare:
A woman with advanced cancer who has been forced to flee to a refugee camp amidst an ongoing civil war
A man with Ebola Virus Disease who has been admitted to a treatment centre at a time when case fatality rates exceed 60%
A child who has suffered a grievous crush injury during an earthquake and is triaged to not receive surgery because others have better chances of survival.
All these individuals require compassionate care to control their symptoms and alleviate their suffering, while considering psychological, cultural, relational and spiritual dimensions of dying. They are illustrative of the wide range of ill and injured persons in humanitarian crises who require palliative care. An approach that the World Health Organisation has defined as “the prevention and relief of suffering by means of early identification and impeccable assessment and treatment of pain and other problems, physical, psychosocial and spiritual.”
Currently, palliative care is the subject of discussion and reflection in many corners of the humanitarian sector. It seems to be accompanying new openness to addressing palliative needs during crises. Smith and Aloudat have advanced the importance of a dual commitment: to promote palliative care but also to challenge inadequate curative treatments available to populations affected by humanitarian crises.
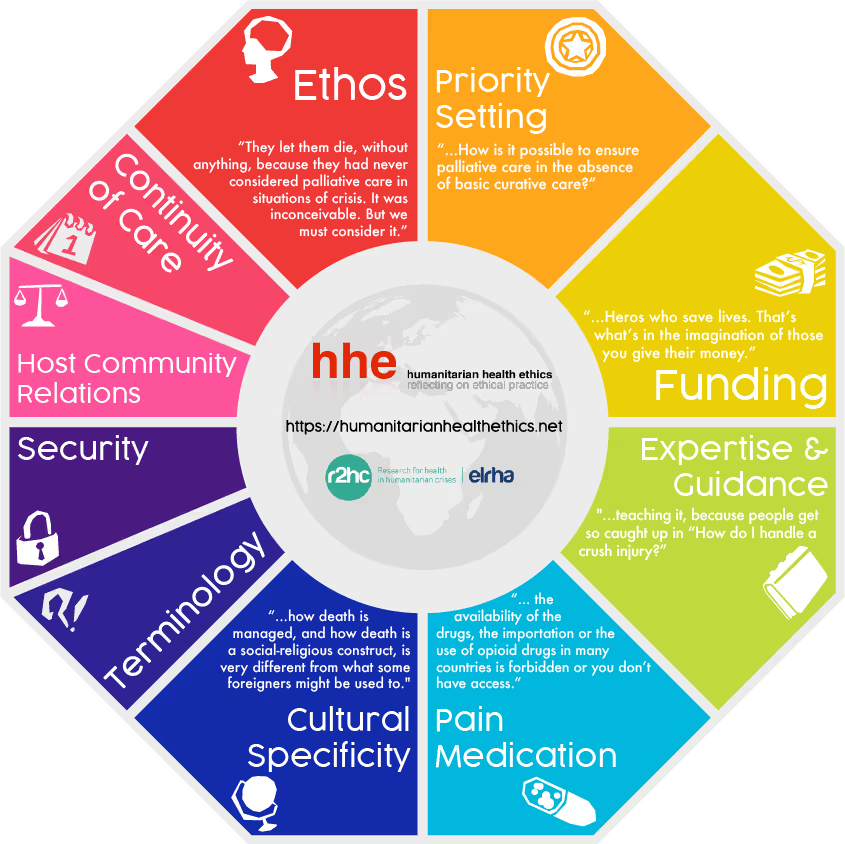
As part of our ongoing R2HC-funded study, we have interviewed humanitarian healthcare professionals and policy-makers about their experiences and perceptions regarding palliative care in humanitarian crises. In this blog, we highlight some of the obstacles that our participants identified as limiting the integration of palliative care in humanitarian healthcare. These obstacles are presented in the accompanying infographic above, along with illustrative quotes from our interviews.
For palliative care to have a place in humanitarian responses these challenges need to be addressed we raise them here to highlight their presence and promote dialogue regarding possible solutions. In a future blog, and as our research project unfolds, we will present and discuss opportunities for overcoming these obstacles.
What are the obstacles to integrating palliative care in humanitarian healthcare?
1.The ethos of humanitarian action
The first obstacle to integrating palliative care discussed by interviewees relates to the ethos of humanitarian action itself, and the primacy given to life saving action. Though humanitarianism’s goals include life saving, alleviation of suffering and promotion of dignity, life saving is the overriding commitment that animates humanitarian healthcare. When lives cannot be saved, this reality may therefore be experienced as a failure of humanitarian actors. This perception, and the overarching focus on life saving, may in turn squeeze out opportunities to address other objectives, including palliative care efforts to ease the suffering of persons who are dying or have life threatening conditions.
2. The need to optimise resources in humanitarian settings
A related consideration is an ethical concern to optimise resources in humanitarian settings. This obstacle is captured by the following position: given the elevated needs and limited resources in acute crises, non-curative actions should only be undertaken once all curative efforts have been implemented. The imperative to rescue, in this sense, is seen by some as always to be prioritised over efforts to alleviate suffering.
3. The need to appeal to donors
Less expected for us were observations that foregrounding palliative care in humanitarian action could make fundraising more difficult. These ideas also echo the issues related to the life saving ethos. Several interviewees suggested that the image of the heroic humanitarian healthcare worker saving lives of injured civilians was expected and seemingly necessary to galvanise support from private donors and large funders alike. Several policy-makers expressed their sense that funding campaigns which include palliative needs of populations are unlikely to be successful.
4. Lack of training and expertise in this area
To date, few organizations have provided training on palliative care or recruited staff who have expertise in this area, leaving humanitarian organizations with limited experience or training in this domain. One element of this situation is that humanitarian medical teams, especially in acute settings, are more likely to include experts in emergency medicine, and trauma and orthopaedic surgery. In other settings, however, humanitarian medical organisations have grappled with providing non-curative care to their patients, most notably in the context of the 2014 Ebola outbreak in West Africa.
5. Barriers to accessing pain medications
Another impediment that looms large in the context of palliative care in many countries are barriers to accessing pain medications such as opiates. Legal and logistical barriers to accessing opioids is a vexing problem in some but not all humanitarian settings. For our interviewees, access to opioids is a necessary, though not sufficient, condition to be able to provide effective palliative care and thus barriers to access were seen as an obstacle to palliative care.
6. Concerns that this care should be provided by local actors
We have also heard reservations expressed about the cultural understanding of humanitarian organisations and many of their staff when they are working in other countries, and whether, therefore, palliative care should be left to local communities and local care providers. It is clearly the case that cultural meanings, practices and expectations associated with death and dying are varied. Humanitarian workers who come from outside a community, especially in an emergency response situation, are unlikely to have in-depth understanding of these considerations.
7. Lack of organisational policies and sector-wide standards
A related obstacle to the lack of training and expertise, is also the lack of organisational policies, and sector-wide standards and guidelines for palliative care during humanitarian crises. While interviewees pointed to examples of new initiatives to establish guidance in this area, they saw the guidance gap as an impediment when field teams were uncertain of how best to respond to the palliative care needs of their patients.
8. Security risks
It was suggested that there may be security risks in providing non-curative care. This concern relates to the possibility that local communities or authorities interpret palliative care efforts as an unwillingness to try to save a loved one or community member. This perception may undermine trust and lead to confrontation.
9. Terminology
Terminology may function as an obstacle for advancing palliative care in some humanitarian organisations. Several interviewees described the term ‘palliative care’ as a source of resistance by some colleagues who were more accepting of the same clinical approaches if other phrasing was employed.
10.Additional challenges include issues ofcontinuity of care and equity between host communities and displaced populations.
These considerations are not unique to palliative care, but present a challenge as humanitarian healthcare organisations strive to expand access to palliative care in contexts where such care is not widely available.
Conclusion
Humanitarian action necessitates confronting care for those for whom curative care is not sufficient, or even possible. As we’ve outlined here, humanitarian health professionals and policy-makers perceive a range of obstacles that exist for integrating palliative care as part of the everyday work of humanitarian health projects. These range from more philosophical considerations, to logistical and legal ones.
Certainly solutions exist, as many of our respondents have also made clear (and which we will discuss in a future post). Overcoming each of these obstacles will require different forms of action both within and beyond humanitarian organisations. Responding to them is vital if humanitarians are to truly fulfil their mandates and commitments not only to attempt to save lives but also to alleviate suffering and promote human dignity. In doing so, some of the most vulnerable recipients can be explicitly recognised and included in the humanitarian response.
Photo Caption: Obstacles to palliative care in humanitarian action. Credit: Humanitarian Health Ethics.
Authors:
Matthew Hunt is an Associate Professor at the School of Physical and Occupational Therapy of McGill University, an associate member of the McGill Biomedical Ethics Unit, and a researcher at the Centre for Interdisciplinary Research in Rehabilitation. He co-leads the Humanitarian Health Ethics Research Group (humanitarianhealthethics.net).
Carrie Bernard is a family physician and palliative lead for the Queen Square Family Health Team in Brampton, Ontario. She is the Associate Programme Director of the Postgraduate Family Medicine programme at the University of Toronto and a member of the Humanitarian Health Ethics Research Group.
Kevin Bezanson is a palliative care consultant for the Northwestern Ontario region
based in Thunder Bay, Ontario, Canada with clinical, research, and programme development experience mainly in Malawi and Ethiopia.Many situations arise in humanitarian crises when curative care is not the primary, or the only, mode for humanitarian healthcare:
A woman with advanced cancer who has been forced to flee to a refugee camp amidst an ongoing civil war
A man with Ebola Virus Disease who has been admitted to a treatment centre at a time when case fatality rates exceed 60%
A child who has suffered a grievous crush injury during an earthquake and is triaged to not receive surgery because others have better chances of survival.
All these individuals require compassionate care to control their symptoms and alleviate their suffering, while considering psychological, cultural, relational and spiritual dimensions of dying. They are illustrative of the wide range of ill and injured persons in humanitarian crises who require palliative care. An approach that the World Health Organisation has defined as “the prevention and relief of suffering by means of early identification and impeccable assessment and treatment of pain and other problems, physical, psychosocial and spiritual.”
Currently, palliative care is the subject of discussion and reflection in many corners of the humanitarian sector. It seems to be accompanying new openness to addressing palliative needs during crises. Smith and Aloudat have advanced the importance of a dual commitment: to promote palliative care but also to challenge inadequate curative treatments available to populations affected by humanitarian crises.
As part of our ongoing R2HC-funded study, we have interviewed humanitarian healthcare professionals and policy-makers about their experiences and perceptions regarding palliative care in humanitarian crises. In this blog, we highlight some of the obstacles that our participants identified as limiting the integration of palliative care in humanitarian healthcare. These obstacles are presented in the accompanying infographic above, along with illustrative quotes from our interviews.
For palliative care to have a place in humanitarian responses these challenges need to be addressed we raise them here to highlight their presence and promote dialogue regarding possible solutions. In a future blog, and as our research project unfolds, we will present and discuss opportunities for overcoming these obstacles.
What are the obstacles to integrating palliative care in humanitarian healthcare?
1.The ethos of humanitarian action
The first obstacle to integrating palliative care discussed by interviewees relates to the ethos of humanitarian action itself, and the primacy given to life saving action. Though humanitarianism’s goals include life saving, alleviation of suffering and promotion of dignity, life saving is the overriding commitment that animates humanitarian healthcare. When lives cannot be saved, this reality may therefore be experienced as a failure of humanitarian actors. This perception, and the overarching focus on life saving, may in turn squeeze out opportunities to address other objectives, including palliative care efforts to ease the suffering of persons who are dying or have life threatening conditions.
2. The need to optimise resources in humanitarian settings
A related consideration is an ethical concern to optimise resources in humanitarian settings. This obstacle is captured by the following position: given the elevated needs and limited resources in acute crises, non-curative actions should only be undertaken once all curative efforts have been implemented. The imperative to rescue, in this sense, is seen by some as always to be prioritised over efforts to alleviate suffering.
3. The need to appeal to donors
Less expected for us were observations that foregrounding palliative care in humanitarian action could make fundraising more difficult. These ideas also echo the issues related to the life saving ethos. Several interviewees suggested that the image of the heroic humanitarian healthcare worker saving lives of injured civilians was expected and seemingly necessary to galvanise support from private donors and large funders alike. Several policy-makers expressed their sense that funding campaigns which include palliative needs of populations are unlikely to be successful.
4. Lack of training and expertise in this area
To date, few organizations have provided training on palliative care or recruited staff who have expertise in this area, leaving humanitarian organizations with limited experience or training in this domain. One element of this situation is that humanitarian medical teams, especially in acute settings, are more likely to include experts in emergency medicine, and trauma and orthopaedic surgery. In other settings, however, humanitarian medical organisations have grappled with providing non-curative care to their patients, most notably in the context of the 2014 Ebola outbreak in West Africa.
5. Barriers to accessing pain medications
Another impediment that looms large in the context of palliative care in many countries are barriers to accessing pain medications such as opiates. Legal and logistical barriers to accessing opioids is a vexing problem in some but not all humanitarian settings. For our interviewees, access to opioids is a necessary, though not sufficient, condition to be able to provide effective palliative care and thus barriers to access were seen as an obstacle to palliative care.
6. Concerns that this care should be provided by local actors
We have also heard reservations expressed about the cultural understanding of humanitarian organisations and many of their staff when they are working in other countries, and whether, therefore, palliative care should be left to local communities and local care providers. It is clearly the case that cultural meanings, practices and expectations associated with death and dying are varied. Humanitarian workers who come from outside a community, especially in an emergency response situation, are unlikely to have in-depth understanding of these considerations.
7. Lack of organisational policies and sector-wide standards
A related obstacle to the lack of training and expertise, is also the lack of organisational policies, and sector-wide standards and guidelines for palliative care during humanitarian crises. While interviewees pointed to examples of new initiatives to establish guidance in this area, they saw the guidance gap as an impediment when field teams were uncertain of how best to respond to the palliative care needs of their patients.
8. Security risks
It was suggested that there may be security risks in providing non-curative care. This concern relates to the possibility that local communities or authorities interpret palliative care efforts as an unwillingness to try to save a loved one or community member. This perception may undermine trust and lead to confrontation.
9. Terminology
Terminology may function as an obstacle for advancing palliative care in some humanitarian organisations. Several interviewees described the term ‘palliative care’ as a source of resistance by some colleagues who were more accepting of the same clinical approaches if other phrasing was employed.
10.Additional challenges include issues ofcontinuity of care and equity between host communities and displaced populations.
These considerations are not unique to palliative care, but present a challenge as humanitarian healthcare organisations strive to expand access to palliative care in contexts where such care is not widely available.
Conclusion
Humanitarian action necessitates confronting care for those for whom curative care is not sufficient, or even possible. As we’ve outlined here, humanitarian health professionals and policy-makers perceive a range of obstacles that exist for integrating palliative care as part of the everyday work of humanitarian health projects. These range from more philosophical considerations, to logistical and legal ones.
Certainly solutions exist, as many of our respondents have also made clear (and which we will discuss in a future post). Overcoming each of these obstacles will require different forms of action both within and beyond humanitarian organisations. Responding to them is vital if humanitarians are to truly fulfil their mandates and commitments not only to attempt to save lives but also to alleviate suffering and promote human dignity. In doing so, some of the most vulnerable recipients can be explicitly recognised and included in the humanitarian response.
Photo Caption: Obstacles to palliative care in humanitarian action. Credit: Humanitarian Health Ethics.
Authors:
Matthew Hunt is an Associate Professor at the School of Physical and Occupational Therapy of McGill University, an associate member of the McGill Biomedical Ethics Unit, and a researcher at the Centre for Interdisciplinary Research in Rehabilitation. He co-leads the Humanitarian Health Ethics Research Group (humanitarianhealthethics.net).
Carrie Bernard is a family physician and palliative lead for the Queen Square Family Health Team in Brampton, Ontario. She is the Associate Programme Director of the Postgraduate Family Medicine programme at the University of Toronto and a member of the Humanitarian Health Ethics Research Group.
Kevin Bezanson is a palliative care consultant for the Northwestern Ontario region
based in Thunder Bay, Ontario, Canada with clinical, research, and programme development experience mainly in Malawi and Ethiopia.
Stay updated
Sign up for our newsletter to receive regular updates on resources, news, and insights like this. Don’t miss out on important information that can help you stay informed and engaged.
Explore Elrha
Learn more about our mission, the organisations we support, and the resources we provide to drive research and innovation in humanitarian response.
%20(3).png)

